Improper Medicare payments down $20.7B since 2014, CMS data show
Fierce Healthcare
NOVEMBER 16, 2021
Improper Medicare payments down $20.7B since 2014, CMS data show. Tue, 11/16/2021 - 07:15.
This site uses cookies to improve your experience. By viewing our content, you are accepting the use of cookies. To help us insure we adhere to various privacy regulations, please select your country/region of residence. If you do not select a country we will assume you are from the United States. View our privacy policy and terms of use.

Fierce Healthcare
NOVEMBER 16, 2021
Improper Medicare payments down $20.7B since 2014, CMS data show. Tue, 11/16/2021 - 07:15.

Healthcare Dive
JUNE 22, 2022
The justices declined to take up the case, leaving intact a lower court ruling that backed the 2014 CMS regulation requiring swift return of overpayments.
This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.

Healthicity
OCTOBER 16, 2023
Medicare Advantage Compliance Under the Spotlight: Lessons from Cigna's $172 Million Settlement $172 million is a lot of money. It's also the amount that the Cigna Group recently agreed to pay to resolve allegations it violated the False Claims Act in relation to its Medicare Advantage (MA) plan enrollees. government joined the action.

Health Law Advisor
FEBRUARY 2, 2023
On February 1, 2023, the Centers for Medicare & Medicaid Services (CMS) published a final rule outlining its audit methodology and related policies for its Medicare Advantage (MA) Risk Adjustment Data Validation (RADV) program. The final rule codifies long-awaited regulations first proposed by CMS in 2018.

Bill of Health
MARCH 24, 2023
The selections feature topics ranging from an analysis of the approval and marketing of biosimilars with a skinny label and their associated Medicare savings, to a discussion of the Philips Respironics recall and the need for reforms to U.S. Characteristics of Prior Authorization Policies for New Drugs in Medicare Part D. 2023 Feb 23.

Healthcare Law Blog
FEBRUARY 1, 2023
On January 30, 2023 , the Centers for Medicare & Medicaid Services (“CMS”) released the long-delayed final rule on risk adjustment data validation (“RADV”) audits of Medicare Advantage (“MA”) organizations (the “Final Rule”). One thing that is certain, CMS can expect further challenges to its RADV audit methodology. 3d 1, 18 n.19

HealthIT Answers
NOVEMBER 14, 2022
By Jordan Rau - The federal government has eased its annual punishments for hospitals with higher-than-expected readmission rates in an acknowledgment of the upheaval the covid-19 pandemic has caused, resulting in the lightest penalties since 2014.

Bill of Health
MAY 22, 2023
The selections feature topics ranging from an analysis of government and industry investments for recently approved drugs, to a discussion of court decisions on mifepristone, and an examination of the added therapeutic benefit associated with the top-selling brand-name drugs in Medicare. Galkina Cleary E, Jackson MJ, Zhou EW, Ledley FD.

Innovaare Compliance
AUGUST 24, 2023
Medicare Advantage plans (MAO) have been increasingly popular with Medicare eligible beneficiaries enrolling 51% of the eligible population in 2023 taking in $454 billion (or 54%) in Medicare spending. MLR measures the percentage of premium income and Medicare payments a Sponsor pays for medical claims.

HIT Consultant
OCTOBER 27, 2023
has seen a consistent decline in primary care clinicians since 2014 due to fewer clinicians entering the workforce, increased rates of burnout and decreased direct patient care, according to the latest evidence report from the Primary Care Collaborative and Robert Graham Center. In 2022, MSSP saved Medicare $1.8

Health Care Law Brief
APRIL 3, 2023
On Friday, March 31, 2023, the Centers for Medicare & Medicaid Services (CMS) released the Calendar Year (CY) 2024 Medicare Advantage (MA) Capitation Rates and Part C and Part D Payment Policies ( Rate Announcement ). 1395w-23): Medicare Advantage Organizations (MAOs) are paid a base rate by CMS. Risk Adjustment.

The Health Law Firm
AUGUST 30, 2013
Board Certified by The Florida Bar in Health Law On August 2, 2013, the Centers for Medicare and Medicaid Services (CMS) released the 2014 Inpatient Prospective Payment System (IPPS) Final Rule (the 2014 IPPS Final Rule). Indest III, J.D.,

Bill of Health
JULY 15, 2022
Potential Medicare Part D Savings on Generic Drugs From the Mark Cuban Cost Plus Drug Company. Medicare Coverage and Out-of-Pocket Costs of Quadruple Drug Therapy for Heart Failure. Post-Marketing Requirements for Cancer Drugs Approved by the European Medicines Agency, 2004-2014. JAMA Netw Open. 2022 Jun 1;5(6):e2216183.

HIT Consultant
MARCH 2, 2023
Centers for Medicare and Medicaid Services (CMS) to continue its work supporting Healthcare.gov. – In 2014, Accenture Federal Services was awarded a prime contract to take over management of the Federally-Facilitated Exchange (FFE).

HIT Consultant
APRIL 11, 2022
Specializing in Medicare Value-Based Care Programs. Vytalize Health started as a Medicare-focused primary care practice in New York in 2014. The company will use the new capital to continue investing in its care delivery infrastructure, partner with Medicare Advantage and commercial plans, and expand its team. ”

VW Health Care Law Blog
NOVEMBER 9, 2016
The Centers for Medicare and Medicaid Services finalized a rule in March 2014 that required healthcare providers prescribing medication, where the prescription is paid for by a Medicare Part D plan, to enroll in Medicare as a prescriber.

HIT Consultant
JULY 14, 2023
FCA Allegations The allegations contends that NextGen falsely obtained certification for its software in connection with the 2014 Edition certification criteria published by HHS’s Office of the National Coordinator. The whistleblowers in this case will receive $5.58M.

The Health Law Firm
FEBRUARY 20, 2016
Circuit ordered the US District Court for the District of Columbia to reconsider a lawsuit seeking to compel the Department of Health and Human Services (HHS) to meet statutory deadlines for reviewing Medicare claims denials. The district court had decided that judicial intervention was not appropriate in such Medicare administrative cases.

Healthcare Law Blog
MAY 16, 2022
On April 29, 2022 , the Centers for Medicare and Medicaid Services (“CMS”), issued the final rule on Contract Year 2023 Policy and Technical Changes to the Medicare Advantage and Medicare Prescription Drug Benefit Programs (the “Final Rule”). With a few exceptions, the Final Rule is a wholesale codification of the proposed rule.

Med-Net Compliance
JULY 20, 2022
A federal jury convicted a New York ENT doctor for defrauding Medicare and Medicaid by causing the submission of false and fraudulent claims for surgical procedures that were not performed. Specifically, between January 2014 and February 2018, the doctor billed Medicare and Medicaid approximately $585,000 and was paid approximately $191,000.

The Health Law Firm
APRIL 21, 2014
Board Certified by The Florida Bar in Health Law For years, the Centers for Medicare and Medicaid Services (CMS) kept private its records on Medicare reimbursement payments made to physicians, however, on April 9, 2014, that all changed. Indest III, J.D.,

HIT Consultant
JUNE 6, 2022
Founded in 2014 by former National Coordinator for Health IT, Farzad Mostashari, Aledade began building ACO networks for independent physicians through the Medicare Shared Savings Program, but now also partners with commercial payers across the country. Delivering Value-Based Primary Care.

The Health Law Firm
JANUARY 13, 2014
Board Certified by The Florida Bar in Health Law The Centers for Medicare and Medicaid Services (CMS) is proposing to exclude providers from Medicare if the government determines a pattern of abusive prescribing practices of Medicare Part D drugs. CMS described these efforts on January 6, 2014, in a proposed rule.

Healthcare IT News - Telehealth
SEPTEMBER 19, 2022
in 2014 and 45.5% Reforming Medicare payment. The study, published in Mayo Clinic Proceedings, found that the prevalence of burnout among U.S. physicians was 62.8% in 2021, compared with 38.2% in 2020, 43.9% in 2017, 54.4% The result is that one in five physicians intends to leave their current practice within two years.
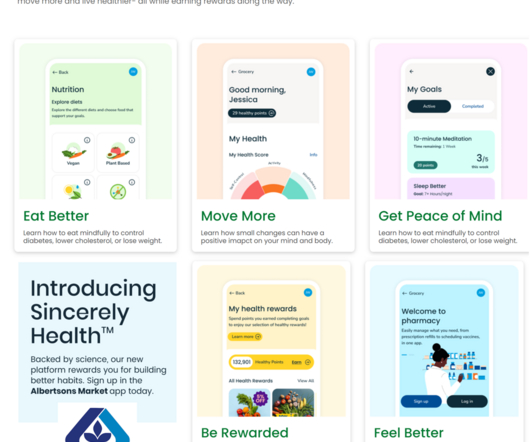
Health Populi
FEBRUARY 21, 2023
This has been a consistent health consumer sentiment for a long time: here’s how I covered PwC’s study on The Wearable Future back in 2014. ” As employers increasingly pay attention to worker wellness and population health, the enterprise-coverage vision that PwC began to quantify in 2014 is (finally) gaining traction.

The Health Law Firm
AUGUST 22, 2016
Board Certified by The Florida Bar in Health Law On July 11, 2016, a federal appeals court stated that a bankruptcy judge did not have the authority to block government health officials from cutting off Medicare and Medicaid payments to a Florida nursing home that was alleged to have violated patient-care regulations. Indest III, J.D.,

The Health Law Firm
DECEMBER 11, 2014
Board Certified by The Florida Bar in Health Law Stop me if you've heard this one before: the Centers for Medicare and Medicaid Services (CMS) recently increased Medicare's authority over physicians and other health care providers. On December 3, 2014, CMS released these new anti-fraud measures. Indest III, J.D.,

Healthcare IT Today
JULY 10, 2023
Company Adds Two Board Members and a Senior Executive to Lead its Medicare Advantage Business Aledade , the largest network of independent primary care practices in the country, today announced the closing of a $260 million Series F funding round to enhance and acquire services and technology to support its practices.

The Health Law Firm
JUNE 4, 2014
The Health Law Firm On June 1, 2015, doctors and other health care providers will be under tighter restrictions when prescribing to Medicare Part D patients. Most health care providers are already enrolled in Medicare. Leider, J.D.,

HIT Consultant
MARCH 20, 2024
The Centers for Medicare and Medicaid Services (CMS) estimated that for payment year 2018 alone , it will recover $428.4 To address these concerns and other matters, CMS announced significant regulatory changes to the Medicare Advantage (MA) program beginning in 2024. million (net) and $4.7

The Health Law Firm
JUNE 6, 2014
Under a rule finalized by the Centers for Medicare and Medicaid Services (CMS) on May 19, 2014, doctors and other health care professionals will be required to enroll in the Medicare program, or have a valid opt-out affidavit on file, for prescriptions to be covered under Part D. By Lance O. Leider, J.D., The Health Law Firm.

Healthcare IT News - Telehealth
DECEMBER 17, 2021
According to the indictment , starting in May 2014 the defendants and their co-conspirators allegedly used telehealth to generate prescriptions for compounded medications and durable medical equipment, regardless of medical necessity.
Healthcare Compliance Blog
MARCH 16, 2022
In a March 11, 2022, release by the Northern District of Georgia’s Office of the Department of Justice, it was reported that an investigation determined a Georgia nursing home knowingly submitted claims for unreasonable, unnecessary, and unskilled services for Medicare patients. This amount was based on the nursing home’s ability to pay.

Healthcare Law Today
JANUARY 11, 2023
The government alleged that, between April 2014 and April 2019, Jet Medical introduced devices into interstate commerce that were misbranded under the Federal Food, Drug and Cosmetic Act (FDCA) because Jet Medical did not obtain approval or clearance from the U.S. and Martech Medical Products Inc.,

Health Care Law Brief
JUNE 26, 2022
Under the traditional, or fee-for-service (FFS), Medicare program, CMS directly pays providers a predetermined rate for the items and services furnished to patients under Medicare Parts A and B. 29844, 29921 (May 23, 2014). CMS’s Payments to MA Plans. at § 1395w-23(b)(4)(D).

Health Populi
JUNE 18, 2021
workers with private insurance more likely report poor access to health care, greater costs of care, and lower satisfaction with care versus people covered by public health insurance plans — whether Medicaid, Medicare, VHA or military coverage. Health Populi’s Hot Points: U.S. households.

Health Law Advisor
FEBRUARY 3, 2022
billion, FY 2021 marks DOJ’s largest annual total FCA recovery since FY 2014, and more than twice the $2.3 Department of Justice (DOJ) released its annual False Claims Act (FCA) enforcement statistics for fiscal year (FY) 2021. [1]. With collections amounting to $5.6 billion received in FY 2020.

Med-Net Compliance
OCTOBER 19, 2022
The settlement resolves allegations that between 2013 and 2020, the company paid remuneration to its home health medical directors in Oklahoma and Texas for the purpose of inducing referrals of Medicare and TRICARE home health patients. The corporate officers were previously the CEO and COO of the company.

Medval Compliance Blog
MARCH 10, 2022
by Frank Fairchok, Vice President of Medicare Reporting Services. Last week, the Centers for Medicare & Medicaid Services (CMS) advanced the rulemaking process in two long-awaited areas. 0938-AT85 – Medicare Secondary Payer and Future Medicals (CMS-6047). 0938-AT85 – Medicare Secondary Payer and Future Medicals (CMS-6047).

Healthcare IT Today
APRIL 21, 2023
Series B funding proceeds will enable Scene to further accelerate its ability to serve Medicaid and Medicare managed care plans, pharmaceutical companies, and clinical research organizations. This financing brings the total investment in Scene to over $25 million since its founding in 2014.

Hall Render
JANUARY 12, 2023
On December 27, 2022, the Centers for Medicare & Medicaid Services (“CMS”) published a proposed rule that could potentially have a significant impact on enrollees’ obligations under the “60-day” overpayment rule. It is not until after this six-month investigation period that the 60 days to report starts to run.

Med-Net Compliance
AUGUST 16, 2022
In addition, from in and around June 2014 to in and around June 2021, the CEO conspired with two regional-level employees and others to commit healthcare fraud. Billing Medicare or Medicaid for services that were not provided is fraudulent activity that is often punishable by fines and imprisonment.

Health Populi
APRIL 8, 2019
That retirement cost gap is the sticker-shock assumption that Medicare is going to cover all health care expenses in retirement. The $285K also assumes the couple doesn’t have employer-sponsored retiree health care coverage and qualifies for “Original Medicare” (not Medicare Advantage, for example).

HIPAA Journal
SEPTEMBER 11, 2023
In 2016, a media outlet reported that members of the health plan were able to access the protected health information (PHI) of other members via the online member portal over a 2-day period in 2014 due to a manual processing error. OCR informed L.A. Care Health Plan it had initiated a compliance review and in February 2016, L.A. The post L.A.
Expert insights. Personalized for you.
We have resent the email to
Are you sure you want to cancel your subscriptions?


Let's personalize your content