Medicare Advantage profitability is declining, Moody’s says
Healthcare Dive
JANUARY 30, 2024
Insurers' MA earnings were 2% lower in 2022 than in 2019, signaling profits in the lucrative insurance program may be weakening.
This site uses cookies to improve your experience. By viewing our content, you are accepting the use of cookies. To help us insure we adhere to various privacy regulations, please select your country/region of residence. If you do not select a country we will assume you are from the United States. View our privacy policy and terms of use.

Healthcare Dive
JANUARY 30, 2024
Insurers' MA earnings were 2% lower in 2022 than in 2019, signaling profits in the lucrative insurance program may be weakening.

Fierce Healthcare
AUGUST 18, 2021
KFF: Medicare Advantage payments increased federal spending by $7B in 2019. Wed, 08/18/2021 - 13:52.
This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.

Healthcare IT News - Telehealth
JUNE 19, 2023
Over the last few years, Medicare Advantage plans have dramatically increased their deployment of telehealth systems for seniors. While some in the healthcare industry may be skeptical of telehealth’s utilization, particularly within the Medicare population, these plans continue to move full steam ahead.

Healthicity
OCTOBER 16, 2023
Medicare Advantage Compliance Under the Spotlight: Lessons from Cigna's $172 Million Settlement $172 million is a lot of money. It's also the amount that the Cigna Group recently agreed to pay to resolve allegations it violated the False Claims Act in relation to its Medicare Advantage (MA) plan enrollees. government joined the action.

Kaiser Health News
JANUARY 28, 2022
A three-judge federal appeals court panel in Connecticut has likely ended an 11-year fight against a frustrating and confusing rule that left hundreds of thousands of Medicare beneficiaries without coverage for nursing home care, and no way to challenge a denial. But it can have serious repercussions.

Healthcare IT News - Telehealth
NOVEMBER 27, 2019
2019: Year in Review It's been an eventful year for health IT. As we look back on 2019, it's worth remembering how far the industry has traveled to get here. -- Mike Miliard, Editor. by Healthcare IT News November 22, 2019. by November 18, 2019. by September 30, 2019. by September 01, 2019.

Electronic Health Reporter
AUGUST 23, 2019
Considering only since the beginning of 2019, the Centers for Medicare and Medicaid Services (CMS) and other federal agencies, such as the Office of National Coordinator of Health IT (ONC) and the Department of Health and […]. One of the greatest challenges in healthcare is keeping up with the changing landscape.

Fierce Healthcare
OCTOBER 19, 2023
billion in savings across 20 of Medicare’s most expensive conditions in 2019— tho | Lobbying groups in favor of overturning the ban on new physician-owned hospitals outlined broad cost savings if 2019's Medicare patients were treated at such facilities instead of a traditional hospital.
HIT Consultant
JANUARY 26, 2023
Mighty Health is the the first all-in-one daily health program designed for adults ages 50 and up—covers more than 9 million Americans nationwide through partnerships with leading Medicare Advantage and commercial health plans. The app has supported more than 200,000 individuals to date, with exciting plans for expansion and new offerings.

Electronic Health Reporter
APRIL 8, 2019
On April 5, 2019, the Centers for Medicare & Medicaid Services (CMS) issued a final rule that updates the Medicare Advantage (MA or Part C) and Medicare Prescription Drug Benefit (Part D) programs by promoting innovative plan designs, improved quality, and choices for patients. Illegal copying is prohibited.

Hall Render
JUNE 8, 2023
On June 7, CMS issued a much-anticipated Final Rule addressing the placement of Medicare Advantage patient days within the Medicare DSH calculation. The Final Rule adopts a retroactive policy that will place Medicare Advantage days in the Medicare Fraction of the DSH calculation for discharges before October 1, 2013.
Kaiser Health News
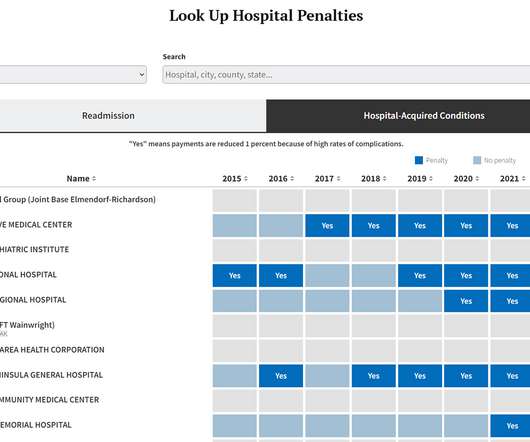
FEBRUARY 8, 2022
The penalties — a 1% reduction in Medicare payments over 12 months — are based on the experiences of Medicare patients discharged from the hospital between July 2018 and the end of 2019, before the pandemic began in earnest. The total amount of the penalties is determined by how much each hospital bills Medicare.

Health Populi
APRIL 8, 2019
The average 65-year old couple retiring in 2019 will need to have a cash nest-egg of $285,000 to cover health care and medical expenses through retirement years, Fidelity Investments calculated. That retirement cost gap is the sticker-shock assumption that Medicare is going to cover all health care expenses in retirement.

Innovaare Compliance
AUGUST 24, 2023
Medicare Advantage plans (MAO) have been increasingly popular with Medicare eligible beneficiaries enrolling 51% of the eligible population in 2023 taking in $454 billion (or 54%) in Medicare spending. MLR measures the percentage of premium income and Medicare payments a Sponsor pays for medical claims.

Electronic Health Reporter
APRIL 7, 2020
The Centers for Medicare & Medicaid Services (CMS) has delivered near $34 billion in the past week to the healthcare providers on the frontlines battling the 2019 Novel Coronavirus (COVID-19). The funds have been provided […].

Bill of Health
MAY 22, 2023
The selections feature topics ranging from an analysis of government and industry investments for recently approved drugs, to a discussion of court decisions on mifepristone, and an examination of the added therapeutic benefit associated with the top-selling brand-name drugs in Medicare. Galkina Cleary E, Jackson MJ, Zhou EW, Ledley FD.

The Health Law Firm
AUGUST 10, 2018
Board Certified by The Florida Bar in Health Law On July 12, 2018, the Centers for Medicare & Medicaid Services (CMS) issued a proposed rule to update payment policies, payment rates, and quality provisions for services rendered under the Medicare Physician Fee Schedule (PFS). Indest III, J.D., Background Info.

Healthcare Compliance Blog
JANUARY 25, 2022
A Missouri woman who had previously pled guilty to Medicare and Medicaid fraud was sentenced in Federal Court to three years imprisonment and ordered to pay $7,620,779 in restitution. Between 2017 and 2019, the Missouri woman owned and managed several durable medical equipment (DME) companies. General Legal Duties and Antitrust Laws.

Healthcare Law Blog
MAY 5, 2022
Department of Health and Human Services Office of Inspector (“OIG”) released a report that studied prior authorization denials and payment denials by Medicare Advantage Organizations (“MAOs”) (the “Report”). Thirteen percent of denied prior authorization requests met Medicare coverage rules. The OIG Report. additional test results).

Hall Render
JULY 18, 2022
The Centers for Medicare & Medicaid Services (“CMS”) has given itself an extra year to review and assess skilled nursing facility proposed regulations issued in 2019. Areas Addressed in 2019 Proposed Rule. Background. Extra Time. The notice extends the timeline to finalize the provisions until July 18, 2023.

Mobi Health News
JULY 12, 2018
The Centers for Medicare and Medicaid Services released its new proposed Physician Fee Schedule and Qualified Payment Program updates for 2019, and the announcement includes some big strides forward in promoting digital health technology, including widened telemedicine coverage, an overhaul of documentation requirements, and a new focus on interoperability. (..)

Health Populi
AUGUST 21, 2019
There are over 60 million enrollees in Medicare in 2019, and fully one-third are in Medicare Advantage plans. Medicare is adding 10,000 new beneficiaries every day in the U.S. Medicare Advantage enrollment is fast-growing, shown in the first chart where over 22 million people were in MA plans in January 2019.

HIT Consultant
DECEMBER 20, 2021
What You Should Know: – Medicare Advantage provider Zing Health raises $25M from Town Hall Ventures and Leavitt Equity Partners, two leading investors focused on growing innovative healthcare businesses.

HIPAA Journal
SEPTEMBER 29, 2022
The Government Accountability Office (GAO) recently conducted a review of Medicare telehealth services provided during the COVID-19 pandemic, when a waiver was in place that greatly expanded access to telehealth and virtual visits. Between April and December 2019, 5 million Medicare telehealth visits were conducted.

Innovaare Compliance
MARCH 1, 2022
The monthly premium for Medicare Part B rose 14.5%, from $148.50 By law, the Medicare Part B monthly premium must equal 25% of the estimated total Part B costs for enrollees age 65 and over. [1] By law, the Medicare Part B monthly premium must equal 25% of the estimated total Part B costs for enrollees age 65 and over. [1]

Health Care Law Brief
APRIL 3, 2023
On Friday, March 31, 2023, the Centers for Medicare & Medicaid Services (CMS) released the Calendar Year (CY) 2024 Medicare Advantage (MA) Capitation Rates and Part C and Part D Payment Policies ( Rate Announcement ). 1395w-23): Medicare Advantage Organizations (MAOs) are paid a base rate by CMS. Risk Adjustment.

Health Populi
OCTOBER 17, 2019
In 2019, it appears that patients have backslid, according to the 2019 Healthcare Consumerism Index from Alegeus. adults in September 2019 on issues concerning health care costs, shopping, value, saving and spending. The first chart shows that the 2019 Index fell from 60.1 points in 2018 to 57.9 households.

Health Populi
APRIL 14, 2019
The post Health/Care Everywhere – Re-Imagining Healthcare at ATA 2019 appeared first on HealthPopuli.com. The barriers to adopting virtual, digital, telehealth modes have been regulatory, financial, and cultural — not so much technical.

Health Populi
JUNE 24, 2019
Cost is the major reason why Medicare Advantage plan beneficiaries switch plans, but people who switch also tend to have lower satisfaction scores based on non-cost factors. Power’s 2019 Medicare Advantage Plan Study. Power surveyed 3,233 members of Medicare Advantage plans in January through March 2019.

Healthcare Law Today
JANUARY 20, 2022
The Centers for Medicare & Medicaid Services (CMS) has responded to these calls by continuing its efforts to address this epidemic and expand access to mental/behavioral health in its new 2022 Physician Fee Schedule Final Rule. The New Rule and the SUPPORT Act. geographic location, originating site, etc.). What’s next?

The Health Law Firm
OCTOBER 31, 2019
Board Certified by The Florida Bar in Health Law On October 1, 2019, a Florida doctor was implicated in what federal investigators say is one of the largest health care fraud schemes ever charged. billion worth of false Medicare and Medicaid claims between July 2018 and January 2019. By George F. Indest III, J.D.,

Hall Render
FEBRUARY 15, 2022
In December 2021, the Office of Inspector General (“OIG”) of the Department of Health and Human Services published an Issue Brief titled “Medicare and Beneficiaries Pay More for Preadmission Services at Affiliated Hospitals Than Wholly Owned Settings” (“Brief”)(available here ). Issue Brief Findings.
Innovaare Compliance
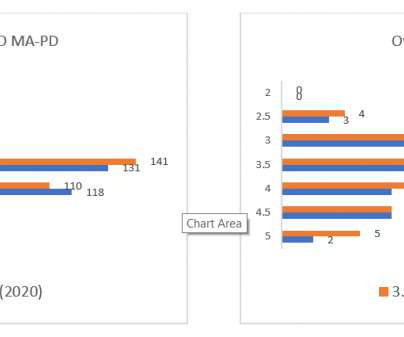
JANUARY 19, 2021
It has become evident by changes to the Centers for Medicare & Medicaid Services (CMS) Star Rating formulas over the past several years—and especially with changes implemented for the 2021 Plan Year—that member experience and medication adherence is of utmost importance to the CMS. Medicare Star Ratings 2021 Changes.

The Health Law Firm
DECEMBER 30, 2019
Board Certified by The Florida Bar in Health Law For years, Florida has topped the lists with the highest rates of Medicare and Medicaid fraud and abuse. But even by the standards of Florida’s rampant healthcare fraud, this 2019 case stands out for its sheer size, making Florida, once again, the leader in fakes and frauds.

Healthcare Law Today
NOVEMBER 9, 2022
Starting January 1, 2023, Medicare will cover telehealth-based treatment services delivered by federally-accredited opioid treatment programs (OTPs), commonly referred to as “methadone clinics.” Background and History of Medicare Telehealth Coverage of SUD Treatment. New Changes to Medicare OTP Telehealth Services.

Healthcare IT News - Telehealth
APRIL 21, 2022
According to a press release , the surgeon, 56-year-old Dr. Elemer Raffai, is accused of allegedly submitting false claims to Medicare in exchange for kickbacks from telemedicine companies. Raffai, together with others, is allegedly connected to the submission of approximately $10 million in fraudulent claims to Medicare.

Healthcare It News
NOVEMBER 23, 2023
It has been working with HSS on the digital transformation of WA Health since 2019. MyMedicare is a voluntary patient registration model launched by the Australian government as part of broader efforts to strengthen the Medicare insurance scheme.

HIT Consultant
OCTOBER 27, 2023
In 2019, there was a net loss of 10 clinicians per 100,000 people across the United States. In 2022, MSSP saved Medicare $1.8 residents currently do not have a relationship with a primary care clinician, and 40% of adults in the United States failed to have a primary care visit in 2019. in 2013 to 4.6%

Healthcare IT News - Telehealth
JULY 22, 2022
Meanwhile, the Centers for Medicare and Medicaid Services' Center for Program Integrity also announced that it has taken administrative actions against more than 50 healthcare providers alleged to be involved in similar schemes. billion in alleged fraud. healthcare system at the expense of patients."

Healthcare IT News - Telehealth
MARCH 25, 2021
Using data from Blue Health Intelligence data repository – an independent data and analytics company that is a licensee of the Blue Cross and Blue Shield Association – researchers from the Johns Hopkins Bloomberg School of Public Health compared claims data from March through June 2019 with March through June 2020.

The Health Law Firm
OCTOBER 3, 2019
Board Certified by The Florida Bar in Health Law On October 1, 2019, a Florida doctor was implicated in what federal investigators say is one of the largest health care fraud schemes ever charged. billion worth of false Medicare and Medicaid claims between July 2018 and January 2019. By George F. Indest III, J.D.,

Healthcare IT News - Telehealth
FEBRUARY 22, 2021
Among the allegations are that Wolfe and her conspirators submitted well over $400 million in illegal durable medical equipment claims to Medicare and the Civilian Health and Medical Program of the Department of Veterans, relying on the guise of "telemedicine" to explain the unusually high volume of claims.

Electronic Health Reporter
MARCH 6, 2020
The Centers for Medicare & Medicaid Services (CMS) took additional actions to ensure America’s patients, healthcare facilities and clinical laboratories are prepared to respond to the 2019-Novel Coronavirus (COVID-19). This article is copyrighted strictly for Electronic Health Reporter. Illegal copying is prohibited.

Healthcare Law Blog
JANUARY 26, 2023
Medicaid and Medicare The Balanced Budget Act of 1997, Public Law 105–33, 111 Stat. The Medicaid and Medicare statutes also contain conscience provisions related to the performance of advanced directives, religious nonmedical healthcare providers and their patients.
Expert insights. Personalized for you.
We have resent the email to
Are you sure you want to cancel your subscriptions?


Let's personalize your content