CMS Imposes New Requirements on Payers to Improve Prior Authorization Process and Payer, Patient and Provider Communications
Hall Render
MARCH 20, 2024
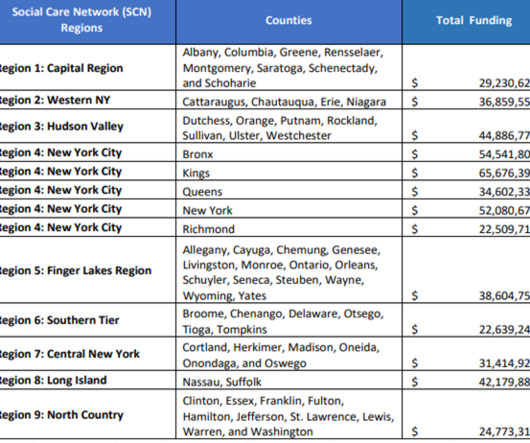
The improved information requirements apply to the following payers, including: Medicare Advantage plans; Medicaid and Children’s Health Insurance Program (“CHIP”) managed care plans; State Medicaid and CHIP fee-for-service payers; and Qualified Health Plans only in the Federally Facilitated Exchanges.
















Let's personalize your content